SUPPORTING CHILDHOOD CANCER RESEARCH

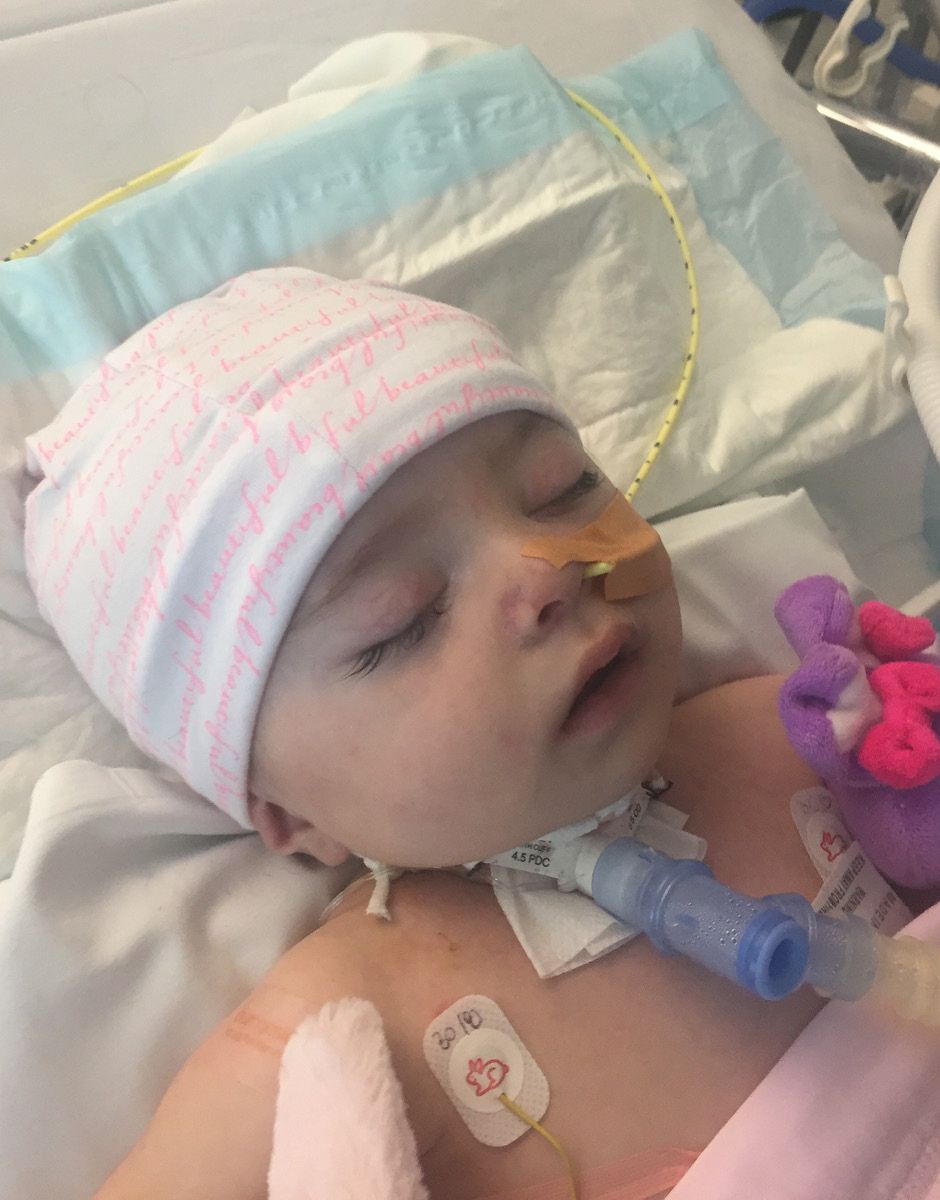
Ellie was just 11-months old when diagnosed with cancer.
We are all too familiar with the hard stories; sick children, brave siblings, and desperate parents. But this is a different story. It’s one of hope, and it’s our best hope yet.
Associate Professor Tracey O’Brien, Director of the Kids Cancer Centre at Sydney Children’s Hospital, Randwick, states three children die from cancer every week in Australia – the equivalent of a classroom of kids every school term.
“I’ve worked in the trenches of childhood cancer for 20 years now,” says Professor O’Brien. “And I can tell you that having a conversation with a parent, telling them that their child may die, and that current treatment offers no hope – it takes a little piece out of you every single time.”
But hope has finally arrived. Zero Childhood Cancer Program is led by Children’s Cancer Institute for laboratory aspects and The Kids Cancer Centre at Sydney Children’s Hospital, Randwick in terms of the clinical facets.
Professor Michelle Haber AM, Executive Director at Children’s Cancer Institute describes it as the most comprehensive children’s cancer personalised medicine program in the world and it’s providing astonishing results.
“The thinking that underpins the Zero Childhood Cancer Program is that every child is unique, their genetic makeup and biology is unique,” says Professor Haber.
“We analyse the genetic and biological characteristics of each child’s tumour and use that information to identify the specific drugs or drug combinations that are most likely [going] to target that child’s individual cancer,” she says.
The Kids’ Cancer Project is proud to be a founding funding partner since 2014 and to date has committed $2,287,250 to the Zero Childhood Cancer Program. The first stage of the program was executed in 2016 with a pilot study for children with high-risk cancer being treated in New South Wales.
After the successful completion of the pilot study in 2017, a national state-of-the-art clinical trial was launched and kids with less than a 30 per cent chance of survival from all over Australia were enrolled on it. Kids like Ellie.
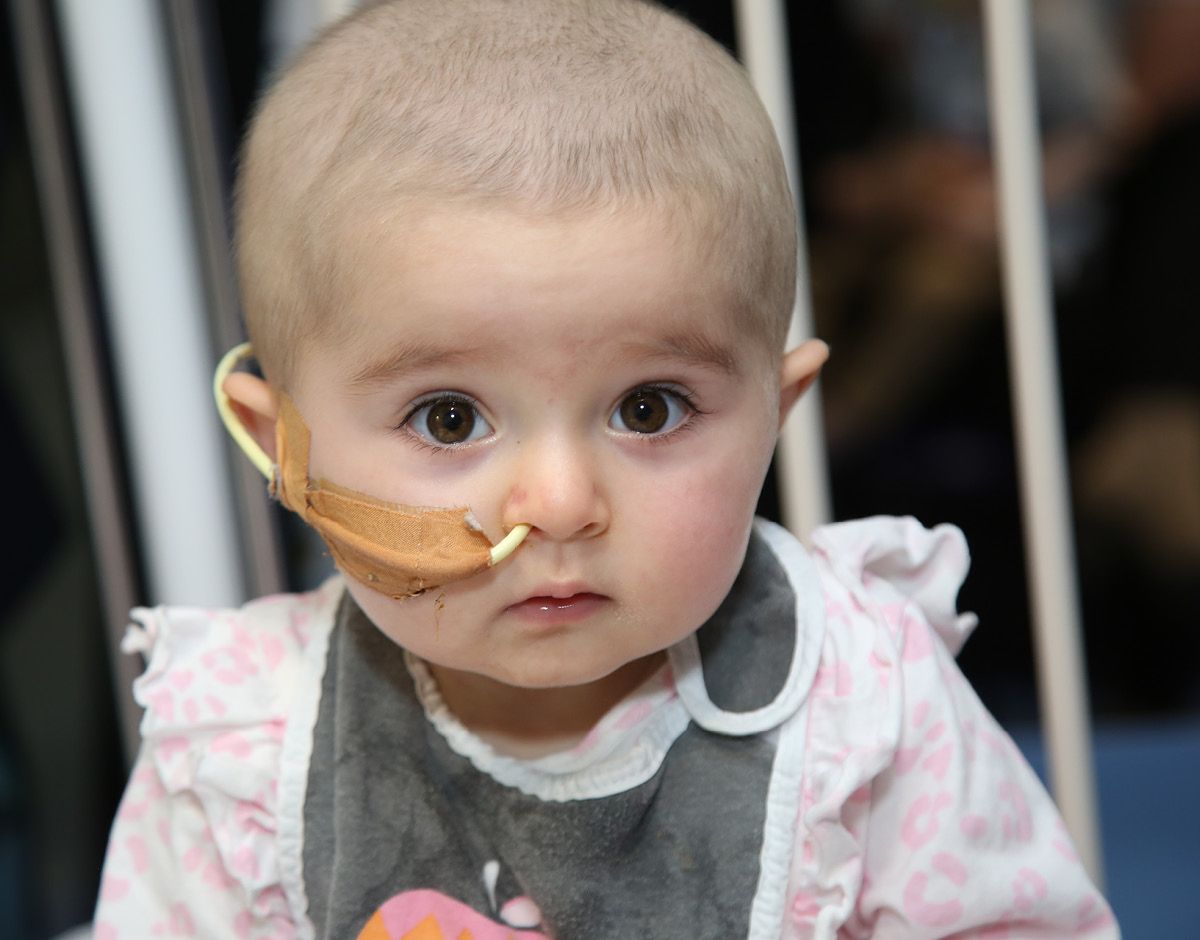
Ellie was enrolled on the Zero Childhood Cancer Program – it saved her life.
Talkative and energetic, three-year-old Ellie is one of the children who have been successfully treated on the program.
Mina and Rob were shocked when at just 11 months of age their little girl, who had been unwell for a couple of weeks, was diagnosed with infantile fibrosarcoma, a rare and aggressive tumour that was resistant to chemotherapy.
“On August tenth, I was on the way to mum’s place to drop Ellie off, and Ellie vomited again, so, I took her to the paediatrician,” says Mina. “He took various tests; x-rays, bloods and he said, “You’ve got a very sick little girl.”
“And then,” says Rob, “It was basically, you need to go to the hospital right now. Not go home. Go straight to the hospital.”
Ellie was admitted to the Kids Cancer Centre at Sydney Children’s Hospital, Randwick under the care of preeminent paediatric oncologist Professor Glenn Marshall AM.
“Within a day of coming to see us at the hospital we had her in the intensive care unit,” says Professor Marshall. “She had a tumour the size of a football on the left side of the chest.”
Ellie’s tumour was so enormous, it was not only pushing on her lungs, it was also pushing her heart out of position. The tiny girl had to be on life support.
“At the time, I thought, I wish we could just take it out. I was prepared as her mother to take it on [myself] because I didn’t want her to endure what she was enduring,” Mina says, her voice cracking with emotion.
“We used chemotherapy in Ellie’s case for two weeks and she had no response,” says Professor Marshall. “In fact, the tumour grew, her condition was worsening by the day and it was essential to find some way of shrinking the mass. Time was running out.”
Professor Marshall met with Mina and Rob to prepare them for the worst, to tell them they needed to say their goodbyes.
“I remember Professor Marshall actually saying to us, ‘she’s hanging on by her ten little fingertips’,” says Mina.
Ellie was enrolled on the Zero Childhood Cancer Program and immediately a dedicated team of doctors and scientists were mobilised. Her tumour DNA was fully sequenced inside of two weeks and the ideal treatment tracked down.
“[The lab] worked day and night around the clock, and we got a result,” recalls Professor O’Brien. “It was a brand new, not described before mutation, and there was a drug that half a dozen children around the world had been treated on – we got that drug here,” she says.
Rob and Mina noticed improvements day by day. After six weeks, the relieved parents were told their baby could come out of ICU and go onto the ward.
“I could see her mouthing words and Rob said, ‘I think she’s trying to say something’,” says Mina. “By October tenth, they decided to take the tracheostomy out and Ellie said, ‘Mama’!
“And she hasn’t stopped talking since,” laughs Rob, and then on a more serious note he continues. “We know that if Ellie had been diagnosed with this cancer even two years ago, she would have died, she is only alive today because of the Zero Childhood Cancer Program.”

Mina, Ellie and Rob will be forever grateful to science and the Zero Childhood Cancer Program.
The extraordinary results even impressed Professor Marshall who, in his long career, has authored more than 160 original research articles on various aspects of childhood cancer.
“It was remarkable actually seeing how much her tumour shrank over a relatively short period and how little the effects of the drug had on her normal tissues,” he says.
“In Ellie’s case, she is in a very good remission however there was significant residual tumour left in her chest cavity,” says Professor Marshall.
“It is important to acknowledge the work of our surgical team in recently cutting out the residual tumour, that still active tumour in it, it was an extremely complex procedure,” he says.
Today, Ellie continues to do well. In 2020, she ‘rang the bell’, signalling her remission. Ellie is now in pre-school and is settling in well. Life is busy, and the family are all happy and healthy.
Together, we can reduce the number of children who die from childhood cancer. Ellie’s case proves it can be done because Zero Childhood Cancer is not just the name of this program, it’s the goal.
- 422 children have been enrolled on the trial, and they have an aggressive cancer that is identified as having less than a 30 per cent chance of survival.
- In terms of cancer types, 36% have brain cancer, 28% sarcoma, 15% leukaemia/lymphoma, 7% neuroblastoma and 14% per cent other rare cancers
- Average turnaround time from receipt of samples to personalised treatment recommendation is under eight weeks
- In October 2020 the first ZERO research paper was published in the prestigious Nature Medicine journal, presenting the findings from the first 250 patients enrolled.
- ZERO identified the molecular, or genetic, basis of a child’s cancer in more than 90% of cases and 70% had at least one new potential treatment option identified based on their cancer’s genetic makeup.
- In the 70% who were recommended a personalised treatment program, at least one, and sometimes several, genetic changes were identified that lead to the potential treatment recommendations.
- 32% of children for whom a therapeutic recommendation was made, received the recommended therapy. The early results of those children showed that in 30% of cases the tumour shrank, and in some patients completely regressed. In another 40% of cases the tumour stopped growing and stabilised.
- In more than 90% of cases the genetic cause of the cancer was identified is important as it provides a way to systematically identify the molecular basis of most childhood cancers.